
On This Page
Latest Stories


To Elevate the Discourse
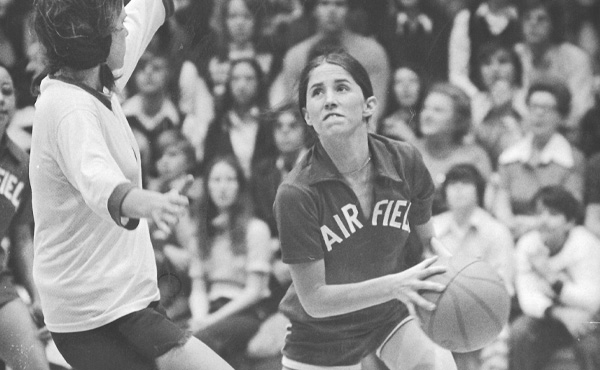
Confident, Courageous, Competitive

The Storm on the Horizon

Taking Care

Anif McDonald ’16

Spring 2024
In this issue, you will find stories about Celebrating a Half-Century of Women’s Athletics, Research by Physics Professor Robert Nazarian, PhD, and his students predicts significant climate changes in northern Mexico — with implications for everyone, A $1.22 million grant will help Fairfield’s midwifery doctoral program in its mission to reduce postpartum mortality in the U.S., and more!Connect With Us
Past Issues
To view a complete archive of past Fairfield University Magazines, please visit digitalcommons.fairfield.edu/fairfield-magazine/.






